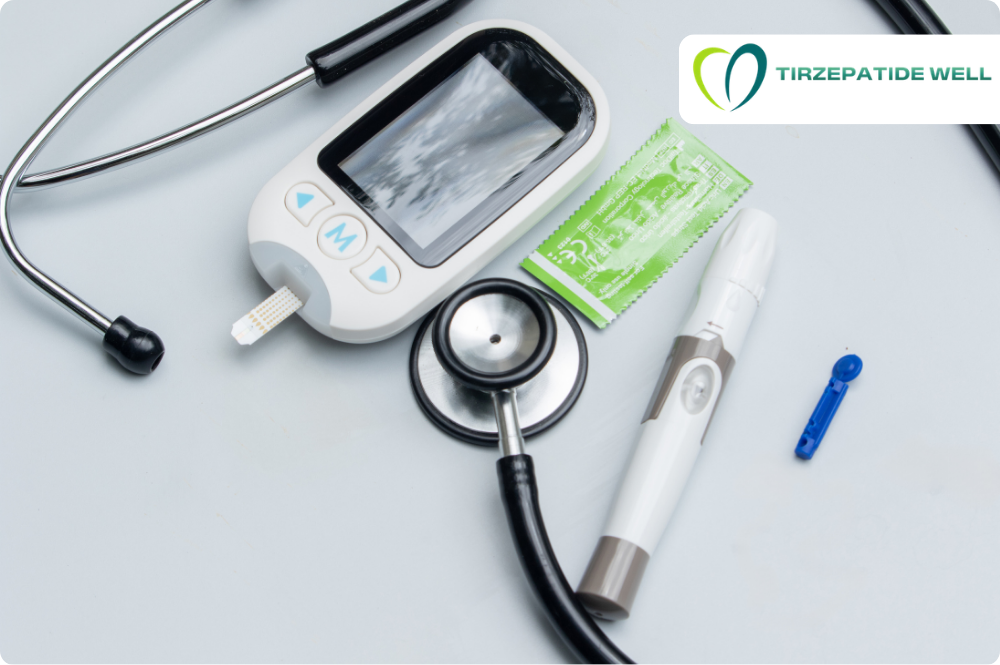
Imagine sitting in your cozy suburban home in the snowy Northeast. You open a letter from your insurance company, and your heart sinks because they said “no” to your medicine. You might wonder, what if insurance denies Tirzepatide coverage, and feel like your weight loss journey is over before it starts.
However, you should know that this happens to many people every single day. Insurance companies have a lot of rules that make it hard to get the help you need. Navigating this confusing medical world is much easier when you have experts to guide you.
Getting a denial letter is frustrating, but it is not the end of the road. There are many ways to get your medicine without having to rely on an insurance company. Let’s look at why they say no and how you can still reach your goals.
Common Reasons for Insurance Denials of GLP-1 Medications
Lack of Prior Authorization
One common reason for a denial is something called Prior Authorization. This basically means the insurance company wants your doctor to ask for permission first. They require a lot of extra paperwork to prove that you really need the medicine.
If the paperwork is not perfect, they will often send a denial letter right away. This can happen even if you live in a busy high-rise in Dallas and have a great doctor. It feels like a lot of red tape just to get healthy.
The “Step Therapy” Requirement
Another tricky rule is called Step Therapy. This is when the insurance company forces you to try older and cheaper drugs first. They want to see if those work before they pay for the better, modern medicine.
Often, these older drugs are not as good for losing weight as Tirzepatide is. It can feel like you are wasting your time on things that don’t help. This rule is a very common reason why people ask What If Insurance Denies Tirzepatide Coverage?
Off-Label Use vs. FDA-Approved Usage
Insurance companies also look closely at why you are taking the medicine. For example, Mounjaro® is approved for diabetes, while Zepbound® is approved for weight loss. If you use one for the other, they might call it “off-label” use.
If your plan only covers diabetes medicine, they might deny your request for weight loss. This is a very common problem for people who are just trying to get their health back on track. It makes the whole process feel much more complicated than it should be.
Step-by-Step: How to Appeal an Insurance Denial
If you get a denial, you can actually fight back by filing an appeal. This means you are asking the insurance company to look at your case one more time. You will need to gather more information and show them why they made a mistake.
First, you should call your insurance company to ask exactly why they said no. Sometimes it is just a simple mistake on a form that can be fixed quickly. Other times, you will need to write a strong letter explaining your health history.
It is very helpful to have expert medical support during this stressful time. A dedicated team like Tirzepatide Well can help you understand the medical side of things. They know the science behind the medicine and can help you navigate the system.
Consider the story of a patient named Sarah who lives in a quiet town in the Midwest. She was denied coverage and felt like giving up on her health goals. However, she found a different path through a telehealth platform that made things simple and affordable.
Get a Tirzepatide Prescription for Weight Loss — 100% Online
Connect with licensed U.S. doctors to start your personalized weight loss journey today. At Tirzepatide Well, we simplify the process with free online consultations from the comfort of your home.
Tirzepatide—the active ingredient in Zepbound® and Mounjaro®—is clinically proven to help patients lose up to 20% of their body weight. We provide medically supervised access to Tirzepatide, Zepbound®, Mounjaro®, Ozempic®, and Semaglutide through trusted physicians.
Affordable and Transparent Pricing Options
Forget the insurance headache. Our program costs $399 per month, covering your prescription, the medication itself, and free home delivery. We also offer Oral Tirzepatide for those who prefer to avoid injections. Our 100% online process is available in all 50 U.S. states, ensuring fast and discreet home delivery for everyone.
Why Choosing a Cash-Pay Telehealth Model Makes Sense
- Price Predictability: You always know exactly what you will pay each month without any surprise bills.
- No Red Tape: You can skip the months of “Step Therapy” and get the medicine that actually works for you.
- Nationwide Availability: You can get care whether you are near the Grand Canyon or living in the Florida Keys.
- Privacy and Comfort: You can talk to a doctor from your own home, no matter the local weather or traffic outside.
When you think about What If Insurance Denies Tirzepatide Coverage?, remember that cash-pay options are often simpler. You get to take control of your own journey without asking for permission. This gives you peace of mind as you work toward a healthier version of yourself.
Comparing Costs: Insurance Co-pays vs. The Tirzepatide Well Model
Some people think insurance is always the cheapest way, but that is not always true. Many insurance plans have very high deductibles that you have to pay first. This means you might pay thousands of dollars out of your own pocket before they help at all.
Even with insurance, your monthly co-pay could be higher than our flat fee. Some plans have a “donut hole” or “gap” where the price suddenly goes up. This makes it very hard to plan your budget and stay on your medicine.
With our $399 flat fee, there are no hidden costs or confusing rules. This is often cheaper than paying full price at a local pharmacy in an expensive city like NYC. You get the medicine, the doctor, and the delivery all for one clear price.
Managing Your Weight Loss Journey Without Stress
Fighting with insurance adjusters can be very bad for your mental health. It adds a lot of stress to a journey that should be about feeling better and getting stronger. Stress can even make it harder for your body to lose weight.
By choosing a predictable monthly plan, you can focus on your habits and your health. You won’t have to spend hours on the phone or wait by the mailbox for a denial letter. You can just focus on the science-backed results and your own progress.
So, What If Insurance Denies Tirzepatide Coverage? You simply choose a path that puts you in charge instead of the insurance company. This allows you to stay consistent with your doses and see the best results possible. Consistency is the most important part of any weight loss plan.
Conclusion: Your Health Shouldn’t Be on Hold
Your health is too important to wait for an insurance company to change its mind. You have the power to find a solution that works for your life and your budget. There are proven ways to get the medication you need without all the red tape.
Whether you are dealing with the humidity in the South or the cold winters of the North, we are here to help. We make sure you can get your medicine delivered right to your door in any of the 50 states. Our goal is to make your journey as smooth and easy as possible.
Even What If Insurance Denies Tirzepatide Coverage? There is a proven, affordable way to continue your journey toward losing 20% of your body weight. You don’t have to let a denial letter stop you from reaching your goals. Take the first step today and see how easy it can be.
Ready to start? Book your free online consultation now and take back control of your health journey.
Authentic Sources and Clinical References
- New England Journal of Medicine (NEJM) – Tirzepatide Study: https://www.nejm.org/doi/full/10.1056/NEJMoa2206038